Understanding Otitis Externa and Indications for Surgery
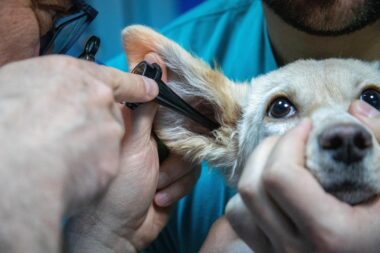
Otitis externa, commonly referred to as swimmer’s ear, is a prevalent ear condition characterized by inflammation of the external ear canal. This condition can result from various factors, including bacterial or fungal infections, allergies, or irritation from water exposure. Patients suffering from otitis externa often experience symptoms such as pain, itching, redness, and discharge from the ear. The anatomy of the ear plays a significant role in understanding this condition, as the ear canal is designed to protect the underlying structures. However, when this protection is compromised, it can lead to infection and an array of complications. Treatment options for otitis externa may range from topical medications to more invasive interventions, depending on the severity of the condition. It’s essential to understand that while mild cases can be treated effectively at home, persistent or severe cases necessitate professional medical attention. If symptoms do not improve with initial treatment, a healthcare provider may recommend further evaluation to determine if surgical intervention is appropriate. Understanding when surgery is indicated is crucial in ensuring effective outcomes and preventing recurrent infections.
One of the primary indicators for considering surgery in otitis externa is the extent of the infection’s severity. In cases where patients do not respond to standard treatments, such as antibiotics or antifungal medications, surgery may become necessary. Surgery can involve debridement of the ear canal, where debris and infected tissue are meticulously removed to promote healing. This procedure aims to restore the ear canal’s natural function and alleviate pain and discomfort experienced by patients. Additionally, if there are anatomical abnormalities, such as a narrow ear canal or bone abnormalities, surgical intervention may be crucial to allowing adequate drainage and preventing future infections. Patients suffering from chronic otitis externa often face repeated attacks of infection requiring ongoing medical care. For these individuals, a surgical approach may offer long-term relief and reduce the likelihood of recurrence. Furthermore, surgery can be particularly beneficial for those whose infections result in complications like abscess formation, which can complicate healing and increase the risk of further issues. Recognizing these indications becomes critical in establishing an effective treatment plan
Another significant factor influencing the decision to pursue surgical intervention in otitis externa is the duration of symptoms. If a patient experiences otitis externa symptoms for more than a few weeks without improvement, surgery may be warranted. Persistent inflammation can lead to chronic changes within the ear canal, potentially resulting in more serious consequences. For example, chronic inflammatory changes can create a conducive environment for the growth of bacteria and fungi, making treatment increasingly complex. Surgical options may involve techniques that facilitate ventilation and drainage within the ear canal, preventing the buildup of moisture that could lead to further infections. This is particularly important for individuals with a history of recurrent infections, as addressing the underlying issue can prevent future occurrences. Additionally, patients experiencing debilitating pain or hearing loss associated with severe otitis externa may find relief through surgical options. These factors highlight the necessity for thorough evaluation and individualized treatment plans tailored to each patient’s unique circumstances and healthcare needs. Empowering patients with knowledge about their options is essential in modern medical care.
Potential Surgical Procedures
When surgery is deemed necessary for otitis externa, several procedures may be considered based on the individual case. One common procedure is myringotomy, which involves making a small incision in the eardrum to relieve pressure and drain fluid. This can be particularly beneficial in cases where the outer ear canal inflammation leads to effusion or fluid buildup. Another option is canalplasty, which refers to the surgical widening of the ear canal to facilitate drainage and prevent recurrence of infections. This procedure often benefits patients with anatomical challenges that predispose them to recurrent otitis externa. In more severe cases, a tympanostomy may be performed, placing a tube in the eardrum to ensure continuous ventilation of the middle ear. Each of these procedures has specific indications, risks, and benefits, which healthcare professionals must carefully consider when discussing surgical options with their patients. It is crucial for patients to engage in open conversations with their healthcare providers regarding their condition and treatment preferences.
Postoperative Care and Recovery
Postoperative care is a vital aspect of recovering from ear surgery related to otitis externa. After any surgical procedure, patients must follow up with their healthcare provider to monitor healing and prevent complications. Patients may experience discomfort or mild pain following surgery, which can be managed with prescribed medications. Additionally, the ear may require special care to ensure that it remains clean and free from moisture during the healing process. Patients are typically advised against activities that could introduce moisture into the ear, such as swimming. Regular follow-up appointments are crucial to evaluate the surgical site and detect any signs of infection early. Depending on the procedure, a healthcare provider may recommend therapies designed to enhance healing and prevent future outbreaks of otitis externa. Education on proper ear hygiene is also important to empower patients in their recovery and mitigate the risk of recurrence. Emphasizing adherence to medical advice during recovery ensures that patients achieve the best possible outcomes from their surgical treatments.
Lastly, understanding the risk factors associated with otitis externa can be highly beneficial in evaluating and managing the condition effectively. Certain individuals may be more prone to developing otitis externa due to various factors, such as living in damp environments, frequent swimming, or having certain skin conditions. It is essential to educate patients about preventive measures to help minimize their risk of developing this condition. Awareness of proper ear care, drying the ears after swimming or bathing, and avoiding the use of cotton swabs can significantly reduce the likelihood of infection. Additionally, individuals should be encouraged to seek prompt medical attention if they exhibit symptoms of otitis externa to ensure timely and appropriate treatment. This proactive approach allows healthcare providers to guide patients through preventive strategies and tailored approaches based on their specific risks. Integrating education on ear health and preventive measures into routine care can promote overall well-being and decrease the incidence of otitis externa for at-risk individuals.
In conclusion, otitis externa is a commonly encountered condition that can lead to various complications and require surgical intervention in severe cases. Understanding the indications for surgery, the procedures available, and the importance of postoperative care can greatly enhance patient outcomes. Continuous education about risk factors and preventive measures also plays a crucial role in managing and preventing recurrent infections effectively. Healthcare providers should foster open communication with their patients to address concerns and empower them to take an active role in their ear health. As research evolves, it is anticipated that new therapeutic strategies and technologies will emerge to improve the management of otitis externa. Patients should remain informed and engaged, seeking care and asking about new innovations that may benefit their health in the context of ear care. Ultimately, a well-rounded approach combining medical and surgical strategies offers the most comprehensive care for individuals experiencing otitis externa and helps ensure long-lasting relief and improved quality of life.
The journey to understanding otitis externa and its treatment options culminates in recognizing the importance of individualized care. Each patient’s experience with otitis externa can vary, carrying distinct personal and medical histories that influence their treatment needs. Professionals in ear care can guide patients to the most appropriate interventions based on specific symptoms and health status. This tailored approach fosters a deeper understanding between patients and their healthcare providers, creating an opportunity for shared decision-making. Furthermore, as we continue to learn about otitis externa and the effectiveness of various treatments, continuous research will enhance medical practices. Patient advocacy programs can also be instrumental in increasing awareness regarding ear health and preventive measures. Ultimately, empowering patients through education and shared decision-making can lead to improved outcomes and satisfaction with care. Engaging in preventative strategies to maintain ear health while also being proactive in seeking treatment when symptoms arise ensures a holistic approach to managing otitis externa. With the right support and resources, patients can navigate their ear health journeys more effectively, embracing a healthier future.